Does TMS Help Anxiety?
Anxiety disorders affect over 40 million adults in the United States, yet many patients remain stuck between partial medication response and ongoing daily impairment. One question increasingly asked in clinics across Texas is: does TMS help anxiety? The short answer is yes—under specific neurobiological conditions and with the right protocol—but understanding why requires a deeper look at brain circuitry, stress hormones, and cortical regulation.
This master guide explains the neuroscience behind Transcranial Magnetic Stimulation (TMS), examines whether TMS is effective for anxiety, and reviews the latest data on TMS success rate anxiety outcomes—while contextualizing access for communities across Texas.
Understanding Anxiety at the Neurobiological Level
Anxiety is not simply “worry.” It is a dysregulation of interconnected neural circuits involving the amygdala, prefrontal cortex, hippocampus, and insular cortex. These regions coordinate threat detection, emotional memory, and executive control.
When functioning optimally, the dorsolateral prefrontal cortex (DLPFC) exerts inhibitory control over the amygdala. In chronic anxiety, functional MRI studies show hyperactivity of the amygdala paired with hypoactivity in the left DLPFC. This imbalance creates a feedback loop where perceived threats are amplified while cognitive regulation is diminished.
The result is persistent sympathetic nervous system activation and elevated cortisol levels. Over time, elevated cortisol can impair hippocampal plasticity, further reinforcing anxiety circuits.
Core Brain Regions Involved in Anxiety
When medications only partially regulate neurotransmitters (like serotonin or norepinephrine), the structural communication between these regions may remain inefficient. This is where neuromodulation enters the conversation.
What Is TMS and How Does It Work?
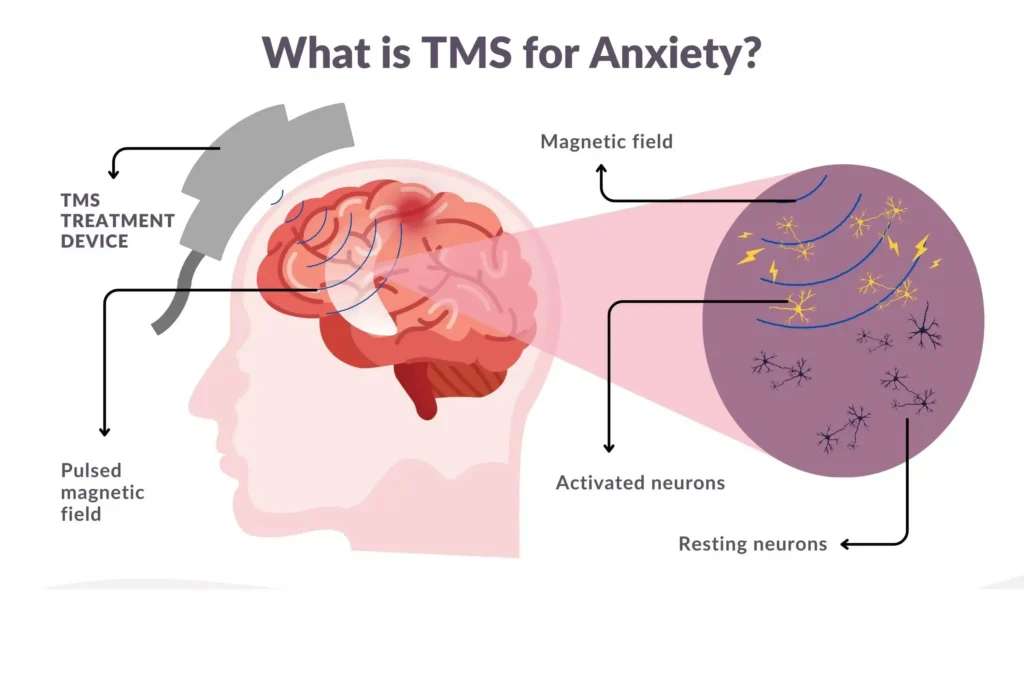
Transcranial Magnetic Stimulation (TMS) is a non-invasive neuromodulation technique that uses focused magnetic pulses to stimulate targeted cortical regions. Most commonly, high-frequency stimulation is applied to the left DLPFC.
Unlike medications that diffuse systemically, TMS directly modulates cortical excitability. Repeated stimulation induces neuroplasticity—specifically long-term potentiation (LTP)—which strengthens underactive circuits.
Mechanism of Action
Does TMS Help Anxiety? The Clinical Evidence
Although TMS is FDA-approved primarily for major depressive disorder, research increasingly supports its use in anxiety-related conditions, especially when anxiety co-occurs with depression.
Meta-analyses show:
- Significant reduction in Hamilton Anxiety Rating Scale (HAM-A) scores
- Improved functional connectivity between DLPFC and limbic regions
- Sustained symptom reduction at 3- and 6-month follow-ups
In patients with treatment-resistant anxiety, response rates range between 50–65%, depending on protocol and diagnostic subtype.
Is TMS Effective for Anxiety Compared to Medication?
Treatment | Mechanism | Response Rate | Side Effects | Long-Term Plasticity |
SSRIs | Serotonin modulation | 40–60% | Weight gain, sexual dysfunction | Limited |
Benzodiazepines | GABA enhancement | Rapid relief | Dependence risk | None |
TMS | Cortical neuromodulation | 50–65% | Mild scalp discomfort | Yes |
Unlike benzodiazepines, TMS does not suppress neural activity globally. Instead, it restores regulatory balance. Compared to SSRIs, TMS offers a non-systemic option without metabolic side effects.
TMS Success Rate Anxiety: What Determines Outcomes?
Success rates vary based on:
- Severity of baseline symptoms
- Comorbid depression
- Duration of illness
- Consistency of treatment sessions
- Coil targeting precision
Patients with high baseline cortisol and measurable DLPFC hypoactivity often show stronger responses. Additionally, combining TMS with cognitive behavioral therapy (CBT) can enhance consolidation of new neural pathways.
Predictors of Strong Response
- Early symptom improvement by week 2
- No benzodiazepine overuse
- Structured sleep patterns
- High treatment adherence
Remission rates may reach 30–40% in carefully selected patients.
Who Is an Ideal Candidate?
TMS may be appropriate for individuals who:
- Have not responded to two or more medications
- Experience intolerable medication side effects
- Prefer non-pharmacological treatment
- Have co-occurring depression and anxiety
However, patients with seizure disorders or implanted metallic cranial devices require careful screening.
Comparing TMS Protocols for Anxiety
Protocol Type | Frequency | Target Area | Best For |
High-Frequency Left DLPFC | 10–20 Hz | Left DLPFC | Anxiety with depression |
Low-Frequency Right DLPFC | 1 Hz | Right DLPFC | Pure anxiety disorders |
Bilateral TMS | Mixed | Both hemispheres | Severe, chronic cases |
Individualized mapping improves precision, particularly in patients with complex symptom profiles.
The Mindful Health Difference: Localized Neuromodulation Across Texas
While understanding the science is critical, outcomes depend heavily on protocol personalization and consistent access to care. That’s where Mindful Health integrates advanced neuromodulation with localized patient-centered delivery across Texas.
Serving the Alamo Heights Community Near The Alamo
In the heart of the Alamo City, patients seeking TMS for anxiety benefit from precise cortical mapping and individualized stimulation parameters. Mindful Health ensures residents near historic landmarks receive evidence-based neuromodulation with physician oversight.
Serving the Bridgeland Community Near Houston Premium Outlets
For Cypress-area residents balancing work along US-290, access to structured TMS sessions improves adherence. Consistency is key to achieving optimal TMS success rate anxiety outcomes.
Strategic Access for the I-35 Corridor Region via Williams Drive
Georgetown patients traveling along the I-35 corridor benefit from coordinated scheduling and minimal disruption to daily routines. TMS sessions typically last 18–30 minutes with no anesthesia required.
Strategic Access for Rockwall County via Interstate 30
Rockwall and Heath residents commuting along I-30 can integrate neuromodulation into weekly care plans without systemic medication adjustments.
Clinical Excellence in the Piney Woods: Solutions for 77301
Conroe-area patients in ZIP code 77301 gain access to advanced TMS technology without traveling to Houston’s urban core.
Clinical Excellence in the Dallas-Fort Worth Lakeside Communities: Solutions for 75032
Heath and Rockwall ZIP 75032 residents benefit from individualized protocols tailored to high-functioning professionals managing anxiety-related executive burnout.
A Localized Standard for Texas Residents
Across San Antonio, Cypress, Georgetown, Rockwall, Heath, and Conroe, Mindful Health provides consistent neuromodulation protocols aligned with emerging psychiatric research. Virtual psychiatric evaluations ensure statewide continuity.
By integrating neuroplasticity science, patient screening, and structured adherence tracking, Mindful Health optimizes outcomes beyond generalized clinic models.
Frequently Asked Questions
- Does TMS help anxiety in San Antonio?
Yes. Mindful Health in San Antonio provides targeted DLPFC stimulation protocols shown to reduce anxiety symptom severity in treatment-resistant cases. - Is TMS effective for anxiety in Cypress, TX?
Mindful Health in Cypress offers evidence-based protocols combining neuromodulation and psychiatric oversight for improved response rates. - What is the TMS success rate anxiety patients see in Georgetown?
At Mindful Health Georgetown, response rates often mirror clinical trial data (50–65%) when patients complete full anxiety treatment courses. - Can TMS replace medication in Rockwall?
At Mindful Health Rockwall, some patients taper medications under supervision after successful neuromodulation. - How long does treatment last in Heath, TX?
Mindful Health Heath typically recommends 5 sessions per week for 4–6 weeks. - Is TMS covered by insurance in Conroe?
Mindful Health Conroe assists with insurance verification and preauthorization. - Does TMS hurt?
Mindful Health clinics across Texas report only mild scalp tapping sensations. - Can anxiety return after TMS?
Mindful Health offers maintenance sessions in San Antonio and other Texas locations if symptoms recur. - Is TMS safe for older adults in Cypress?
Yes. Mindful Health Cypress screens patients carefully for safety and contraindications. - Do I need a referral in Georgetown?
Mindful Health Georgetown provides psychiatric evaluations to determine candidacy without requiring external referral.Conclusion: A Data-Driven Path Forward
Anxiety is rooted in measurable neurocircuit dysregulation involving the amygdala and DLPFC. TMS directly addresses this imbalance through cortical stimulation and neuroplastic remodeling. Evidence suggests meaningful improvement in 50–65% of treatment-resistant cases, with remission possible in a significant subset.
For Texas residents seeking a structured, science-based solution, Mindful Health delivers precision neuromodulation across San Antonio, Cypress, Georgetown, Rockwall, Heath, and Conroe. By combining advanced cortical targeting with localized access and insurance coordination, Mindful Health transforms the question from “does TMS help anxiety?” into “how soon can we begin restoring balance?”